You can read a little bit about my initial diagnosis of Hallux Limitus. After quite a lot of research on the different stages of this condition and the options I decided I was a good candidate for a Cheilectomy surgery. The limited range of motion of my big toe was bothering me, I was noticing an increased pain level in various activities from walking to putting on ski boots. A Cheilectomy is a good intervention for early to mild Hallux Rigidus and given I want to keep hiking pain-free for many years I decided to follow up with my orthopedic surgeon who I had been working with. Read on for details of my Cheilectomy surgery for Hallux Limitus!
After some discussion and more research I decided to go ahead with this surgery. The surgeon looked favorably on this and the recovery time. The recovery time was my biggest concern as I want to be able to continue with my JMT hike in the summer. We scheduled the surgery for mid-Feb but then had to reschedule for early March after an ice storm came through Portland the day before the initial surgery. As some background, I have never had surgery before. So all this was new to me, hopefully, it will help other folks through the procedure.
This posting contains details of the first week after surgery – be warned there are some graphic photos here.
Day of Surgery – 9th March 2021
I arrived at the hospital at 10 am. As far as I could tell the operation would take about 60-90 minutes and would roughly start at 12pm. I’d expect to be on my way home at around 2.30 pm.
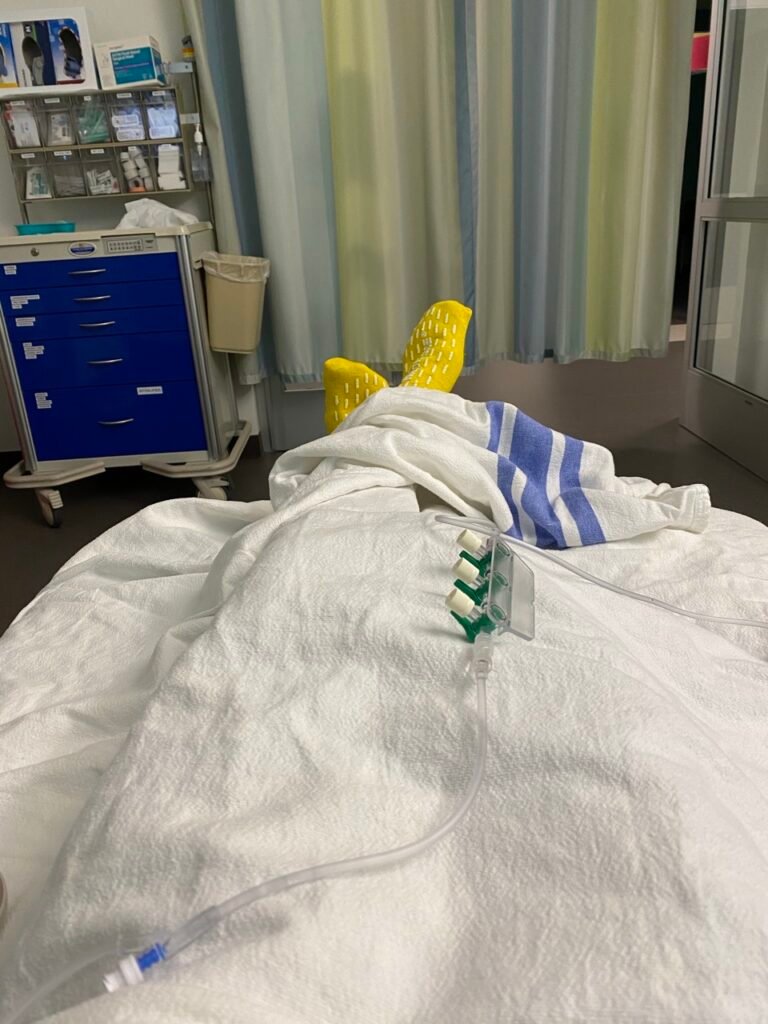
Shortly after arriving a nurse showed me to a pre-op room, this must have been shortly after 10 am. The first hour was pretty slow. I changed into a surgical gown, and rested on a bed, covered in a blanket. A lot of medical questions around medical history etc., but also a lot of waiting. Blood pressure taken (127/95) – surprised it wasn’t higher considering, heart rate and temperature. A nurse placed an IV in the back of my right hand – which was no different from a normal injection.
At around 11 am things got a little busier. The resident came along and basically outlined the rest of the process. Talked a little bit about the anesthesia, and an overview of the operation. He verified some basics medical information, which foot would be operated on, and clearly marked that foot with a marker pen. We chatted about the actual operation and how they would basically chisel away some bone and file down what’s left. Basically, orthopedics is metalwork tools on your bones!
Just before the anesthesia team arrived they wanted me to go to the bathroom. I hadn’t eaten or drank anything for over 11 hours. Going to the bathroom with an IV and gown is a bit of a hassle and probably not the most dignified experience – but overall hospitals and dignity don’t seem to go hand in hand.
Anesthesiology
One of the anesthesiologists, Lori, arrived and started to talk about the option and procedure. In all fairness, there were not really any options at this point and this is one area I wish I had discussed in a little more detail in advance. What had been recommended was a nerve block for my foot and a light general anesthetic. Lori also described some mild sedatives to help me relax during the preparation. Suddenly the room was full of about 5-6 people, including the surgeon. A lot of conversations going on. Another anesthesiologist, Dr. Lopez, who was going to administer the nerve block came in and started a conversation. Double checked on the limb etc, He started to prep my left leg, which required me to shift to resting on my right side.
At about this time, Lori said she’d administer a sedative and I might feel a little bit of cold at the IV site. Sure enough, it did and then waited a couple of seconds before asking the fateful question of “How long does it take before this works”. Which were basically the last words I remember before waking up in the recovery room.
I am assuming that I was not unconscious at all at that point (not really hooked up to any of the right equipment). And that would happen later in the OR. So for quite a period of time, I was conscious and responding to questions and conversations and have absolutely no recollection. I have a very vague recollection of seeing briefly the inside of the OR. The next thing I remember is waking up in the recovery room. That’s definitely a bit spooky. Given the completeness of the nerve block – I wonder whether just having that as a local anesthetic would have been enough.
I did ask and received photos from the actual surgery. To me these are fascinating but if you don’t like to see the inside of your body don’t follow this link.
Immediate Recovery
I think I was awake in the recovery room at about 2 pm. Again I remember having some fairly lucid conversations. The memory of the details is very thin. Drank some coffee (already missing not having coffee in the morning). The surgeon and resident came by and said all went well. And then my wife appears. There’s some more conversation which luckily my wife was more engaged with on post-op care. A final visit to the restroom, apparently a prerequisite, and then discharged.
Pain, or lack there off
After the operation, my foot was still numb from the nerve block. It was completely numb. We were sent home with a prescription for Oxycodone. With a recommendation to take one at night if the block had not worn off. This was to help prevent not waking up in the middle of the night. My foot was well bandaged and in a boot.
Even after the block had worn off there was really minimal pain. The block took a full 24 hours to wear off. This was right at the long end of how long it was supposed to last. It’s fair to say I was getting a little worried at the 24-hour mark. But shortly after I was able to move a toe a little bit and then over the next 2-3 hours, it wore off completely.
Midday on Wednesday I took one Oxycodone, with the expectation of pain getting worse. But it generally didn’t and that was the only one I took. I haven’t need any other pain management so I’ve been very happy from that perspective. In fact, the most irritating aspect has been a sore throat from the tube used to keep my airways open during surgery. That was like having a sore throat for 3 days.
Surgical Summary
I took a look at the medical reports that were posted as part of my medical record. I guess all went well as the only things that were really mentioned were that the anesthesia process was “easy” and “patient tolerated surgery well”.
Immediate post operative recovery – first week
So far the only real post-operative instructions are to keep my foot above my heart to minimize post-operative swelling. This basically means spending a lot of time on my back with my leg raised. I can’t tell if there is any swelling. My foot is dressed and there doesn’t seem to be any indication of bleeding.
I returned to work the next day – Covid helped here as I was working from home here anyway. And this just meant working from home, on my back. Not as productive, harder to type – but not too bad.
Walking required crutches for the first day – just because my left foot was still numb. As soon as the nerve block wore off I could move onto ‘Heel walking’ in the boot. Not a hugely efficient way of getting around.
I can move my big toe a little without pain. Its range of motion is clearly very limited because of the dressing. But it actually feels pretty good.
The next real milestone is on the 22nd of March. That is the post-operative follow-up and when the stitches will be removed and I can really start working on the physical therapy side.
So far I’m very happy with the medical side, the operation, support staff, and information were all top-notch.







Following your ‘adventure’. I think you are about 1 “step” ahead of me.
I’m using a full carbon insole in my hiking boots, walking with Hoka Bondi 7, and use Birkenstocks with a bunch of carbon strips duct taped to the front to limit flexing. Getting by with that.
Did my first microspike hike a couple days ago. They work fine but the elastic presses down on the big toe joint and after that goes on for a couple hours it got pretty sore.
Trying figure out what is the most productive next move is for me. Hope not to give up an entire season, at least not this year.